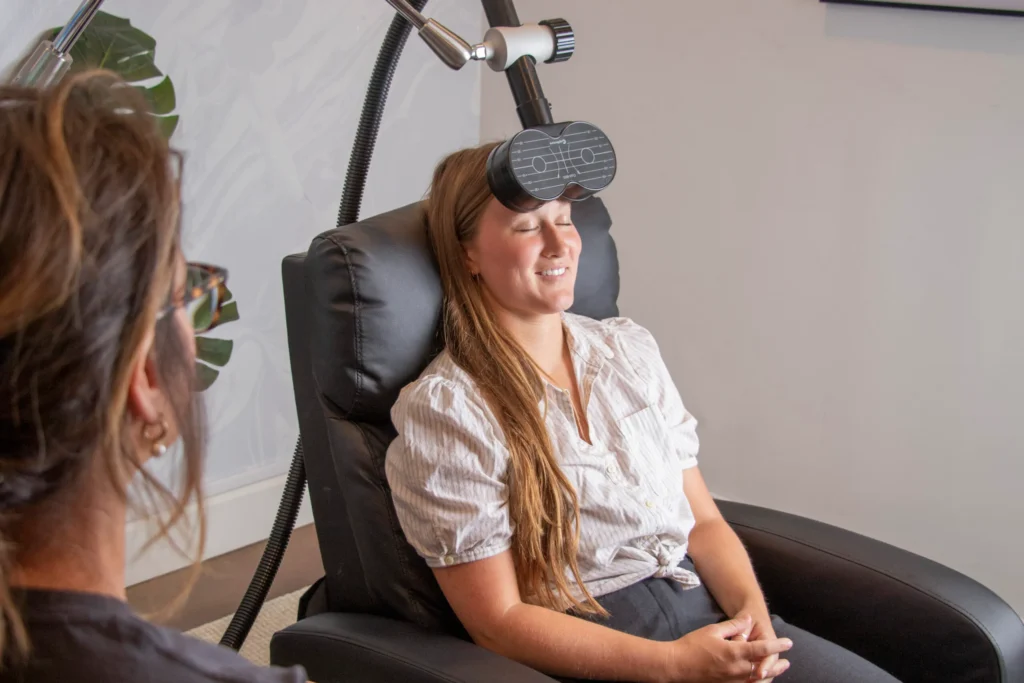
Using a magnetic coil, Transcranial Magnetic Stimulation (TMS) delivers targeted pulses to specific areas in the brain, boosting the neural activity in under-active areas. In the past few years, TMS has exploded in popularity due to its efficacy in treating conditions such as OCD, PTSD, and depression. Efficacy rates for TMS are known to be above 85% in some clinics. Remission rates (no symptoms of depression) can be as high as 65%. But what often gets overlooked is the importance of supporting the benefits of the treatment with talk therapy.
TMS is a robust treatment, but the most effective and meaningful change comes from combining it with evidence-based talk therapies such as Cognitive Behavioral Therapy (CBT) or Exposure Response Prevention (ERP).
Why Combine the Two?
Think of TMS addressing the biological side of mental health – improving your brain function and mood.
However, with mental health, there are the psychological and behavioral aspects, and those changes come from talk therapy sessions. Within these sessions, the thoughts, habits, and emotional responses are addressed, and behavioral changes are made.
It is similar to the idea of working out – you lift weights to build muscle, then take supplements and protein powder to lock in the progress from the gym. Similarly, TMS is rewiring your brain circuitry, and therapy sessions support and cement behavioral changes with your newly trained brain.
OCD: Why TMS Still Requires ERP
Obsessive-compulsive disorder is a condition where uncontrollable, recurring thoughts (obsessions) and repetitive behaviors (compulsions) decrease the afflicted individual’s quality of life.
TMS can help target the hyperactivity in the brain that is associated with OCD, which helps to calm the recurring thoughts. To help with the compulsions of OCD, it is important to learn how to respond differently to the thoughts.
This is where therapy plays its biggest role – modalities such as Exposure Response Prevention are a great tool for treating OCD.
Exposure and response prevention works by having an individual repeatedly face their fears and being trained to face them without performing their compulsions. The fear is consistently exposed until it eventually extinguishes, and the individual no longer feels the desire to perform their rituals.
Combining the two treatments is the most effective way to treat the two components that entail OCD.
PTSD: TMS Can Help – But Trauma Work is Still Necessary
Post-traumatic stress disorder (PTSD) is caused by an extremely stressful event that results in flashbacks, nightmares, high anxiety, and negative mood.
TMS helps target the anxiety and depressive components of PTSD. The root cause of the disorder is unresolved memories from the stressful event. This is where therapies such as Eye Movement Desensitization and Reprocessing (EMDR) help.
EMDR uses guided eye movements to help the brain process distressing memories in a safer, more positive way. This helps reduce the emotional intensity of the memory, making it feel less painful.
TMS helps stabilize the chemicals in the brain, while therapy will help target the root cause of PTSD.
Depression and TMS: The Effective Therapeutic Approaches for Long-lasting Change
TMS is most heavily used for depression, as it helps increase the brain activity in underactive areas, overall leading to mood improvements.
Talk therapy is a powerful tool that can provide long-lasting change and prevent cases of relapse. It can help patients make healthier decisions, develop healthier relationships, or learn to manage conflict. Therapeutic approaches such as CBT, thought field therapy (TFT), and psychodynamic are great examples. For many patients, a course of TMS is a chance to start life over with a positive mood and mindset. A therapist can help patients decide how they want to maintain and move forward with a new beginning.
Combining both TMS and talk therapy modalities is the best way to help make the most impactful change to effectively treat depression.
Esha Nushrat is a pre-medical student interested in Neurology. She has been working in mental health for the past two years as a TMS technician. She is an advocate for mental health and volunteers at organizations such as Stride in Recovery and NAMI.
Dr. Thomas Hughes is an adolescent and adult interventional psychiatrist. He is the owner and founder of Seen Medical and NeoPsych in Glendale, CA. He specializes in medication management and Transcranial Magnetic Stimulation for depression, anxiety, OCD, and PTSD.
NeoPsych
213-433-2823
Seen Medical
www.seenmedical.com/psychiatry
213-433-2823

Dr. Thomas Hughes is an adolescent and adult interventional psychiatrist. He is the owner and founder of Seen Medical and NeoPsych in Glendale, CA. He specializes in medication management and Transcranial Magnetic Stimulation for depression, anxiety, OCD, and PTSD.